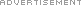Breast Augmentation Complications – Double Bubble, Tuberous Breasts & More
Reviewed by Walter Erhardt, MD
Breast augmentation can be a complex surgery, and complications may occur. More invasive surgery can mean more risk, and longer breast augmentation recovery time. As a general rule, the more invasive a procedure is, the greater the risk.
Before you have breast enlargement surgery, discuss possible complications with a board-certified plastic surgeon who has experience performing breast augmentation. Risk can be reduced by choosing a skilled, experienced plastic surgeon to perform the procedure and by carefully adhering to the surgeon’s instructions, both before and after the surgery.
Some breast augmentation risks include:
- Infection
- Asymmetry
- Bottoming Out
- Double Bubble
- Capsular Contracture
- Anaplastic Large Cell Lymphoma
Infection
If infection occurs, it’s usually within days or weeks of surgery. In rare cases infection can occur long after breast surgery — even when the incisions are completely healed. The earlier an infection is diagnosed and treated, the better the outcome. In severe cases it may be necessary to remove the implant until the infection subsides. (It can be replaced at a later date.)
Asymmetry
Asymmetrical (uneven) breasts can occur following breast augmentation for a variety of reasons, including uneven healing. One solution is fat transfer breast augmentation, which uses injections of your own fat to make your breasts appear more symmetrical. This procedure can also be used after breast reconstruction, for the treatment of tuberous breasts or for a modest (less than one cup size) enhancement.
Tuberous Breasts
Tuberous breast deformity is a congenital condition in which the breasts fail to fully develop. Women with this deformity have breasts that are long and narrow with tight skin below the nipple and enlarged areolas. In some cases, the nipples and areolas may stick out.
Tuberous breast deformity can range from mild to severe. The cause of this condition is unknown. However, it can be corrected with several types of breast enhancement surgery.
During areolar incision surgery, your surgeon crafts an around-the-areola incision and then makes several incisions within the breast to release the tight breast tissue. This treatment is sometimes combined with breast augmentation with implants or a breast lift.
The procedure is usually performed while you are under general anesthesia at an outpatient surgical facility. It typically takes two hours or more to complete, but this will depend upon the extent of the surgery and whether breast lift or breast implants are included.
Following surgery, expect to wear surgical dressings and a compression garment for several days. Any stitches are removed within a week’s time. Light activities can then be resumed, but strenuous activities should be avoided for three weeks.
Patience is required, as it takes some time for the breasts to expand to a more natural, rounded appearance.
The cost of tuberous breast surgery is difficult to estimate due to the many variables involved (such as whether breast implants or breast lift is included). Insurers do not cover tuberous breast correction because it is not considered a medically necessary procedure. The best way to find out how much tuberous breast correction will cost is to consult with a board-certified plastic surgeon. The surgeon will examine your breasts, assess your general health and discuss your goals. Based on this information, he or she will provide you with an estimate.
Bottoming Out
Bottoming out is a complication that occurs when the implant rides too low in the breast tissue, causing the nipple to point upwards. Correction for bottoming out involves breast augmentation revision surgery that re-creates the pocket(s) within the breast that holds the implant(s).
Double Bubble
“Double bubble” is a descriptive term for a postsurgical complication that can occur after breast augmentation with breast implants. Specifically, double bubble happens when an implant drops down behind the natural fold (inframammary crease) where the lower breast meets the chest, rather than forward into the breast. This shifting creates an unnatural indentation or line across the bottom (lower pole) of the breast; this is particularly visible when the arms are lifted above the head. When viewed in profile, double bubble is said to have a “four-breast effect.”
Fortunately, double bubble is a relatively rare complication that is correctable in most cases.
Causes of Double Bubble
There are several scenarios that can result in double bubble, including improper breast implant placement. Double bubble occurs most often in women with sagging breasts whose implants were placed under the chest (pectoral) muscles. (This placement is known as submuscular, and the implants are referred to as “unders.”) The breast tissue hangs low enough to look like one set of breasts. The implants look like another.
The risk of this occurring may be reduced by placing the breast implants over the muscle. (This is known as a subglandular placement, and the implants are referred to as “overs.”) Alternatively, the surgeon may recommend that the woman have both a breast augmentation and a breast lift.
Double bubble can also happen after pregnancy. This occurs when breast tissue droops from the excess weight gained during pregnancy, but the implants remain where they were originally placed.
Also at high risk are women who have limited lower breast skin, or a short distance between the bottom of the areola (dark skin around the nipple) and the breast crease.
Another contributing factor for double bubble is breast augmentation capsular contracture. This occurs when scar tissue tightens around the implant, causing aesthetic and physical problems.
Capsular contracture occurs most often during the first two years following breast augmentation recovery.
Double bubble can also occur when:
- Implants are too big (heavy) for the chest wall and cause the supporting tissues to stretch, settle or migrate below the inframammary crease
- Implants are poorly positioned by the surgeon
- The mammary crease is constricted
- The woman has tuberous breasts
- Scarring is present from previous breast surgeries
Double bubble can develop at almost any time after breast augmentation surgery. If you develop this complication, consult with your surgeon. Remedies do exist.
Correcting Double Bubble
There are several ways to correct double bubble, all of which involve surgical intervention.
One option is revision breast augmentation surgery involving a breast lift (mastopexy) and submuscular placement of the implants.
Another corrective action for double bubble involves removing the implants and placing new ones in front of the muscle. This placement can fill out sagging skin, but rippling may occur.
Alternatively, the breast crease can be modified. A small incision is made in the crease, which is then tightened and raised by placing sutures along the bottom of the breast. This eases the implant back into its proper position.
The right double bubble correction for your situation should be determined during a consultation with your original plastic surgeon. If your breast augmentation was recent (within the past six months), your surgeon may advise a “wait and see” approach to determine if it improves on its own. If you’re farther out from your original surgery date, you may need revision surgery. Depending on your surgeon’s revision policy, you may not have to pay his or her surgical fee, although you will still be responsible for the anesthesia and facility fees.
Alternatively, you can choose another qualified plastic surgeon to perform the revision. Be sure that he or she is a board certified plastic surgeon who has extensive experience performing double bubble surgery and breast augmentation revision.
Start your search for the right surgeon now.
Synmastia
Synmastia refers to the breasts being too close to each other. Surgery may be needed to correct synmastia.
Capsular Contracture
Capsular contracture, or breast hardening, can occur anytime after surgery, typically within a few months. A capsule created by scar tissue compresses the implant, causing it and the breast to look distorted. In the most advanced cases, the implant can feel hard and misshapen. The implant itself has not changed or hardened, but the capsule squeezing the implant has caused it to feel as though it has. Visit our article on capsular contracture for more detailed information on this complication.
Anaplastic Large Cell Lymphoma
Breast implants may increase a woman’s risk for a rare blood cancer called anaplastic large cell lymphoma (ALCL). So far there have been 60 reported cases of ALCL among 5 to 10 million women with breast implants worldwide. Though small, this number is striking given the rarity of this cancer. The Food and Drug Administration is now creating a national registry of ALCL cases linked to breast implants. This cancer does seem to be less aggressive when linked to breast implants than when found in the absence of implants. Treatment often only entails breast implant removal. Symptoms may include pain, swelling, asymmetry and/or lumps. Talk to your breast surgeon, gynecologist or primary care doctor if you are concerned about your risk for ALCL. For the latest information, visit our article on ALCL and breast implants now.
Additional Considerations
In addition to the possible complications listed above, there are a number of additional considerations that should be part of the conversation when considering breast augmentation. These considerations include:
Breast-Feeding
Many women with breast implants can breast-feed, but in some cases breast implants may interfere with breast-feeding.
Discuss your thoughts about breast-feeding with your plastic surgeon in advance of your surgery date. This information may affect your choice of incision and implant placement. For example, a periareolar incision (around the edge of the nipple) may disturb your milk ducts. In addition, placing implants below the chest muscle is least likely to disturb the milk ducts and may be an option if you plan to breast-feed. Be open with your surgeon regarding your future plans and desires.
Mammography
Breast implants can make it slightly more difficult to read a mammogram. This should not be taken as a reason to skip your annual breast cancer screening exam. Mammograms are the best way to detect breast cancer when it is in its earliest and most treatable stages. This is true regardless of whether or not you have breast implants.
Additional views called Eklund displacement views may be required if you have breast implants. Tell the personnel at the breast imaging center about your implants when you make the appointment so they can schedule the extra time for Eklund displacement views.
Your plastic surgeon may be able to refer you to a center that sees many women with breast implants. Remind the technician about your breast implants at the time of your mammogram. On rare occasions, mammograms may cause implant rupture.
Loss of Sensation
After breast surgery with implants, you may experience some loss of sensation in your nipple and breast area. This results from damage to nerve endings in the breast and nipple. The loss of sensation may become permanent. Certain breast augmentation techniques may confer a higher risk of this complication than others. Your surgeon can determine the most appropriate implant type and surgical technique to reduce your risk of this breast sensitivity side effect.
Leaking or Leaching of Breast Implant Material
If a saline breast implant leaks, the saltwater solution is seamlessly and harmlessly absorbed by your body. If a silicone gel-filled breast implant leaks, local complications such as hardening or scarring of breast tissue may occur. There is, however, no risk of the silicone gel migrating outside of the breast and causing systemic disease.

Rupture
Breast implants can break or rupture, resulting in deflation. Ruptures can occur for many reasons, including the natural aging of the implant, excessive compression or trauma to the breast. If rupture occurs, the size and shape of your breast may change. Typically, implant removal with replacement or another type of surgery is required if your breast implant ruptures.