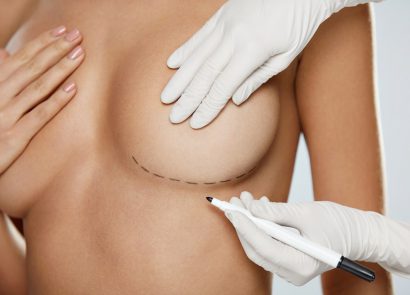
Breast Augmentation
Plastic Surgery Pavilion
5441 Far Hills Avenue
Dayton, OH 45429
(800) 736-1729
Learn More
Raj Plastic Surgery
The Atrium
30400 Detroit Rd #LL10
Westlake, OH 44145
440-808-8030
Learn More
Totonchi Plastic Surgery
2500 MetroHealth Drive
Cleveland, OH 44109
216-778-4450
Learn More
29017 Cedar Road
Lyndhurst, OH 44124
(440) 461-7999
Learn More

Breast Augmentation

Body Contouring
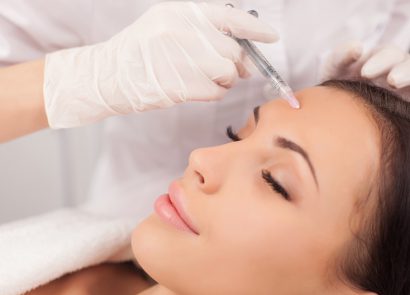
Injectables & Fillers

Anti-aging
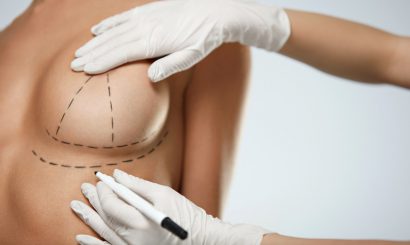
Breast lift

Breast Implants

Breast Implants

Hair Transplants
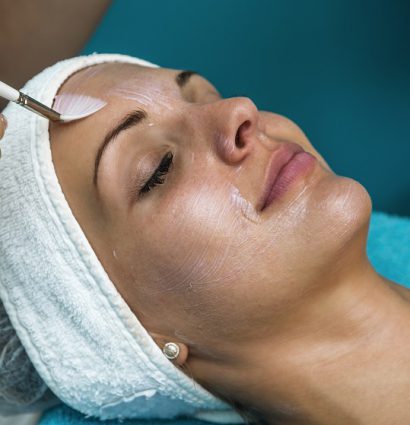
Facial Rejuvenation

Eyes
Breast Implants
Skin
Injectables & Fillers

Rhinoplasty

Breast Implants